- Clinical Study
- Comparison of the Efficacy and Safety of Insulin Detemir Administered Once Daily According to Two Titration Algorithms (3-0-3 and 2-4-6-8) in Patients with Type 2 Diabetes Mellitus
-
Hea Min Yu, Kang Seo Park, Jun Hwa Hong, Keun Yong Park, Jong Min Lee, Bon Jeong Ku, Yeo Joo Kim, Tae Kun Oh
-
Endocrinol Metab. 2020;35(1):142-148. Published online March 19, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.1.142
-
-
4,761
View
-
80
Download
-
3
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
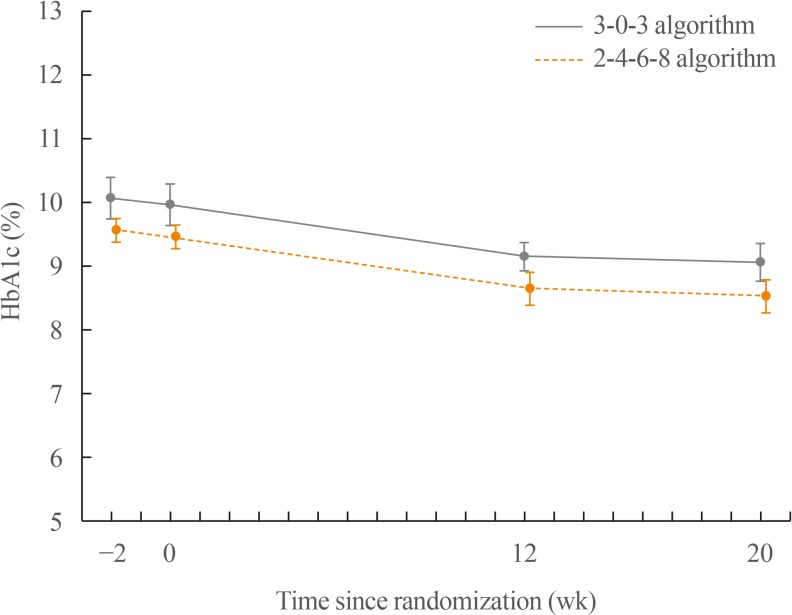
This study was conducted to compare glycaemic control with insulin detemir administered according to two titration algorithms (3-0-3 and 2-4-6-8) after 20 weeks of treatment in subjects with type 2 diabetes mellitus inadequately controlled on metformin. MethodsThis was a 20-week, randomised, multicentre, open-labelled, treat-to-target trial. Forty-six patients were randomised in a 1:1 manner to either the 3-0-3 (G3, n=23) or 2-4-6-8 (G2, n=23) algorithm. The primary endpoint was change of haemoglobin A1c (HbA1c), and the secondary safety endpoint included hypoglycaemic events. ResultsAfter 20 weeks, HbA1c decreased similarly in the G3 and G2 groups, with a mean change of −0.9% from baseline. The mean change in fasting plasma glucose was numerically similar in both groups. The hypoglycaemia event rate per 100-patient-years of exposure (r) in the G2 group (r=1,427) was higher than that in the G3 group (r=807). ConclusionBoth treatment groups had numerically similar HbA1c reductions. A trend towards fewer hypoglycaemia episodes after dose stabilisation was seen with the simpler G3. Clinically, this may be an important observation, as a simpler titration algorithm may support self-management and maintenance of insulin therapy.
-
Citations
Citations to this article as recorded by  - Time for Using Machine Learning for Dose Guidance in Titration of People With Type 2 Diabetes? A Systematic Review of Basal Insulin Dose Guidance
Camilla Heisel Nyholm Thomsen, Stine Hangaard, Thomas Kronborg, Peter Vestergaard, Ole Hejlesen, Morten Hasselstrøm Jensen
Journal of Diabetes Science and Technology.2022; : 193229682211459. CrossRef - Efficacy and safety of patient-led versus physician-led titration of basal insulin in patients with uncontrolled type 2 diabetes: a meta-analysis of randomized controlled trials
Marco Castellana, Filippo Procino, Rodolfo Sardone, Pierpaolo Trimboli, Gianluigi Giannelli
BMJ Open Diabetes Research & Care.2020; 8(1): e001477. CrossRef
- Thyroid
- Papillary Thyroid Carcinoma: Four Cases Required Caution during Long-Term Follow-Up
-
Hea Min Yu, Jae Min Lee, Kang Seo Park, Tae Sun Park, Heung Young Jin
-
Endocrinol Metab. 2013;28(4):335-340. Published online December 12, 2013
-
DOI: https://doi.org/10.3803/EnM.2013.28.4.335
-
-
3,816
View
-
28
Download
-
3
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
Due to the increased prevalence of papillary thyroid carcinoma (PTC), difficult cases and unexpected events have become more common during long-term follow-up. Herein we reported four cases that exhibited poor progress during long-term follow-up. All the cases were diagnosed with PTC and treated with total thyroidectomy before several years, and the patients had been newly diagnosed with recurrent and metastatic PTC. These four cases included recurred PTC with invasion of large blood vessels, a concomitant second malignancy, malignant transformation, and refractoriness to treatment. Physicians should closely monitor patients to promptly address unforeseen circumstances during PTC follow-up, including PTC recurrence and metastasis. Furthermore, we suggest that the development of a management protocol for refractory or terminal PTC is also warranted. -
Citations
Citations to this article as recorded by  - Induction of epithelial-mesenchymal transition in thyroid follicular cells is associated with cell adhesion alterations and low-dose hyper-radiosensitivity
Ankit Mathur, Vijayakumar Chinnadurai, Param Jit Singh Bhalla, Sudhir Chandna
Tumor Biology.2023; 45(1): 95. CrossRef - Thyroglobulin Level in Fine-Needle Aspirates for Preoperative Diagnosis of Cervical Lymph Node Metastasis in Patients with Papillary Thyroid Carcinoma: Two Different Cutoff Values According to Serum Thyroglobulin Level
Min Ji Jeon, Won Gu Kim, Eun Kyung Jang, Yun Mi Choi, Yu-Mi Lee, Tae-Yon Sung, Jong Ho Yoon, Ki-Wook Chung, Suck Joon Hong, Jung Hwan Baek, Jeong Hyun Lee, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Thyroid.2015; 25(4): 410. CrossRef - Brief Review of Articles in 'Endocrinology and Metabolism' in 2013
Won-Young Lee
Endocrinology and Metabolism.2014; 29(3): 251. CrossRef
- Thyroid
- Graves' Disease that Developed Shortly after Surgery for Thyroid Cancer
-
Hea Min Yu, Soon Hyun Park, Jae Min Lee, Kang Seo Park
-
Endocrinol Metab. 2013;28(3):226-230. Published online September 13, 2013
-
DOI: https://doi.org/10.3803/EnM.2013.28.3.226
-
-
3,176
View
-
31
Download
-
7
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
Graves' disease is an autoimmune disorder that may present with various clinical manifestations of hyperthyroidism. Patients with Graves' disease have a greater number of thyroid nodules and a higher incidence of thyroid cancer compared with patients with normal thyroid activity. However, cases in which patients are diagnosed with recurrence of Graves' disease shortly after partial thyroidectomy for thyroid cancer are very rare. Here we report a case of hyperthyroid Graves' disease that occurred after partial thyroidectomy for papillary thyroid cancer. In this case, the patient developed hyperthyroidism 9 months after right hemithyroidectomy, and antithyroglobulin autoantibody and thyroid stimulating hormone receptor stimulating autoantibody were positive. Therefore, we diagnosed Graves' disease on the basis of the laboratory test results and thyroid ultrasonography findings. The patient was treated with and maintained on antithyroid drugs. The mechanism of the recurrence of Graves' disease in this patient is still unclear. The mechanism may have been the improper response of the immune system after partial thyroidectomy. To precisely determine the mechanisms in Graves' disease after partial thyroidectomy, further studies based on a greater number of cases are needed. -
Citations
Citations to this article as recorded by  - Graves’ disease diagnosed in remnant thyroid after lobectomy for thyroid cancer
Meihua Jin, Ahreum Jang, Won Gu Kim, Tae Yong Kim, Won Bae Kim, Young Kee Shong, Min Ji Jeon, Byeong-Cheol Ahn
PLOS ONE.2022; 17(3): e0265332. CrossRef - Graves’ thyrotoxicosis soon after hemithyroidectomy for low-risk papillary thyroid carcinoma
Ahmad Housin, Michael Tamilia
BMJ Case Reports.2022; 15(5): e250149. CrossRef - Effects of energy-based ablation on thyroid function in treating benign thyroid nodules: a systematic review and meta-analysis
Yuan Fei, Yuxuan Qiu, Dong Huang, Zhichao Xing, Zhe Li, Anping Su, Jingqiang Zhu
International Journal of Hyperthermia.2020; 37(1): 1090. CrossRef - Total Thyroidectomy for Thyroid Cancer Followed by Thyroid Storm due to Thyrotropin Receptor Antibody Stimulation of Metastatic Thyroid Tissue
Lars Folkestad, Frans Brandt, Thomas Brix, Marianne Vogsen, Lars Bastholt, Peter Grupe, Jeanette Krogh Petersen, Laszlo Hegedüs
European Thyroid Journal.2017; 6(5): 276. CrossRef - Percutaneous microwave ablation of thyroid nodules: effects on thyroid function and antibodies
Kristina Heck, Christian Happel, Frank Grünwald, Huedayi Korkusuz
International Journal of Hyperthermia.2015; 31(5): 560. CrossRef - Development of Thyroid-Associated Ophthalmopathy in Patients Who Underwent Total Thyroidectomy
Sun Young Jang, Ka Hyun Lee, Jong Rok Oh, Bo Yeon Kim, Jin Sook Yoon
Yonsei Medical Journal.2015; 56(5): 1389. CrossRef - Brief Review of Articles in 'Endocrinology and Metabolism' in 2013
Won-Young Lee
Endocrinology and Metabolism.2014; 29(3): 251. CrossRef
- A Case of Complete Agenesis of the Dorsal Pancreas in a Patient with Newly Diagnosed Diabetes Mellitus.
-
Dong Pil Kim, Kang Seo Park, Dong Sun Kim, Bong Suk Ko, Ji Hae Lee, Jae Hyuk Lee, Jong Ho Shin, Byung Jun Kim, Hyun Jin Kim
-
J Korean Endocr Soc. 2010;25(1):78-83. Published online March 1, 2010
-
DOI: https://doi.org/10.3803/jkes.2010.25.1.78
-
-
 Abstract Abstract
 PDF PDF
- Agenesis of the dorsal pancreas is a rare congenital anomaly caused by underdevelopment or agenesis of the dorsal pancreatic bud that forms the upper head, neck, body and tail of the pancreas. We report a case of agenesis of the dorsal pancreas, which was found under examination of diabetes mellitus (DM). A 16-year-old girl was transferred to our hospital because of a positive urine glucose reading during a school-conducted examination. Abdominal computed tomography and magnetic resonance cholangiopancreatography revealed the deficit of the pancreatic body and tail. Diabetes-associated autoimmune antibodies were negative in a blood test. Decreased beta-cell function was demonstrated by oral glucose tolerance and glucagon stimulation tests. Although the notion that agenesis of the dorsal pancreas leads to decreased endocrine or exocrine function is controversial, the results of this study suggest that we should consider these causes of diabetes mellitus. When treating a young patient with diabetes mellitus, we should consider causes of diabetes mellitus such as congenital anomaly or maturity onset diabetes, in addition to type 1 and type 2 diabetes mellitus.
- A Case of Systemic Lupus Erythematous (SLE) with Graves' Desease and Idiopathic Thrombocytopenic Purpura (ITP).
-
In Sung Cho, Kang Seo Park, Young Cheol Kim, Kyung Il Chun, Sook Kyung Hong, Hyun Choi, Jae Ryong Han
-
J Korean Endocr Soc. 1997;12(4):677-683. Published online January 1, 2001
-
-
-
 Abstract Abstract
 PDF PDF
- Autoimmune diseases are occasionally associated with other autoimmune diseases in the same patients. Autoimmune Graves' disease has been associated with systemic rheumatic diseases including systemic lupus erythematosus (SLE). And Graves' disease associated with idiopathic thrornbocytopenic purpura (ITP) has been reported many times in Korea. There is a special relationship between SLE and ITP, both of which are autoimmune diseases. Some patients with thrombocytopenic purpura, labeled as idiopathic at the onset, later develop a classical course of SLE, suggesting that ITP may be an early manifestation of SLE. The relationships among these three conditions and their pathogenesis are poorly undemtood, and the coexistence of these diseases at the same time has been reported very rarely, but it may be very probable that there are some relationships among them. We report a case of SLE associated with Graves' disease and ITP treated well by imunosup-pressive agent who had been suffering from recurrence by conventional treatments (antithyroid medication, corticosteroid, subtotal thyroidectomy and splenectomy).
- A Case of Addison's Disease: Partial Recovery of Adrenocortical Function Following Antituberculous Medication.
-
Kang Seo Park, Jong Il Jun, Kyung Keun Cho, Mi Sook Kim, Jin Man Huh, Man Soon Baek, Moon Jun Na
-
J Korean Endocr Soc. 1997;12(4):642-646. Published online January 1, 2001
-
-
-
 Abstract Abstract
 PDF PDF
- Addisons disease is relatively rare than secondary adrenal insufficiency and result from progressive adrenocortical destruction. The common causes are idiopathic autoimmune atrophy and tuberculosis of adrenal glands. It is generally regarded as incurable in the sense that substitution therapy is required for the rest of the patients life. We report a case of tuberculous primary adrenal insufficiency which was confirmed by biopsy. This case was treated with antituberculous medication and showen to have improved adrenocortical function after six months.
- A Case of Isolated ACTH Deficiency Accompanied by hyperprolactinemia.
-
Young Seung Kim, Gwang Il Kim, Dae Su Kim, Jeon Ok An, Sang Jeong Yoon, Hee Cheol Jang, Kang Seo Park
-
J Korean Endocr Soc. 1997;12(3):462-467. Published online January 1, 2001
-
-
-
 Abstract Abstract
 PDF PDF
- Isolated ACTH deficiency is a uncommon disorder causing secondary adrenocortical insufficiency. Less than 200 cases have been reported in the world. The major clinical manifestations are hypoglycemia, weight loss, hypotension, anemia, weakness, nausea, inability to excrete water load, and hyponatremia. A 56-year-old male was admitted because of weakness, fatigue, nausea and vomiting. He was pallor and not associated with hyperpigmentation. The basal plasma ACTH and cortisol levels were 8.30 pg/ml and 0.6 ug/dl. The serum cortisol did not response to rapid ACTH stimulation test. On combined pituitary stimulation test, the cortisol did not response to insulin-induced hypoglycemia. Other anterior pituitary hormones showed normal responses except elevated prolactin level. Six months after glucocorticoid replacement therapy, the elevated basal prolactin level returned to normal. Brain MRI did not show any anatomic abnormalities of the sellar and suprasella area. We report a case of isolated ACTH deficiency accompanied by hyperprolactineia, which respond to glucocorticoid replacement therapy.
|